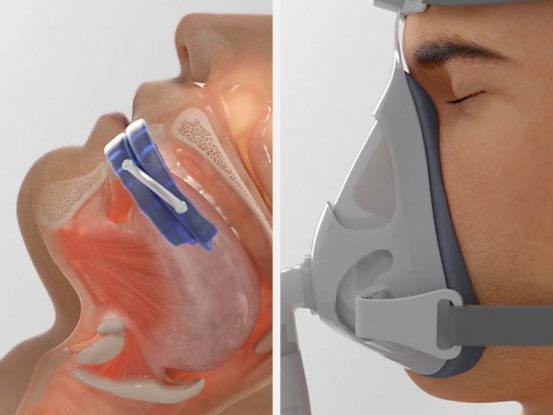
Did you know a common root cause of snoring is your tongue?
eXciteOSA for snoring tones your tongue with NMES therapy, a clinically proven approach to reduce snoring and improve the quality of your sleep.1-3
A simple 20 minute-a-day therapy with nothing to wear at night.

Are you a candidate for eXciteOSA?
Clinically proven to reduce snoring in just 6 weeks

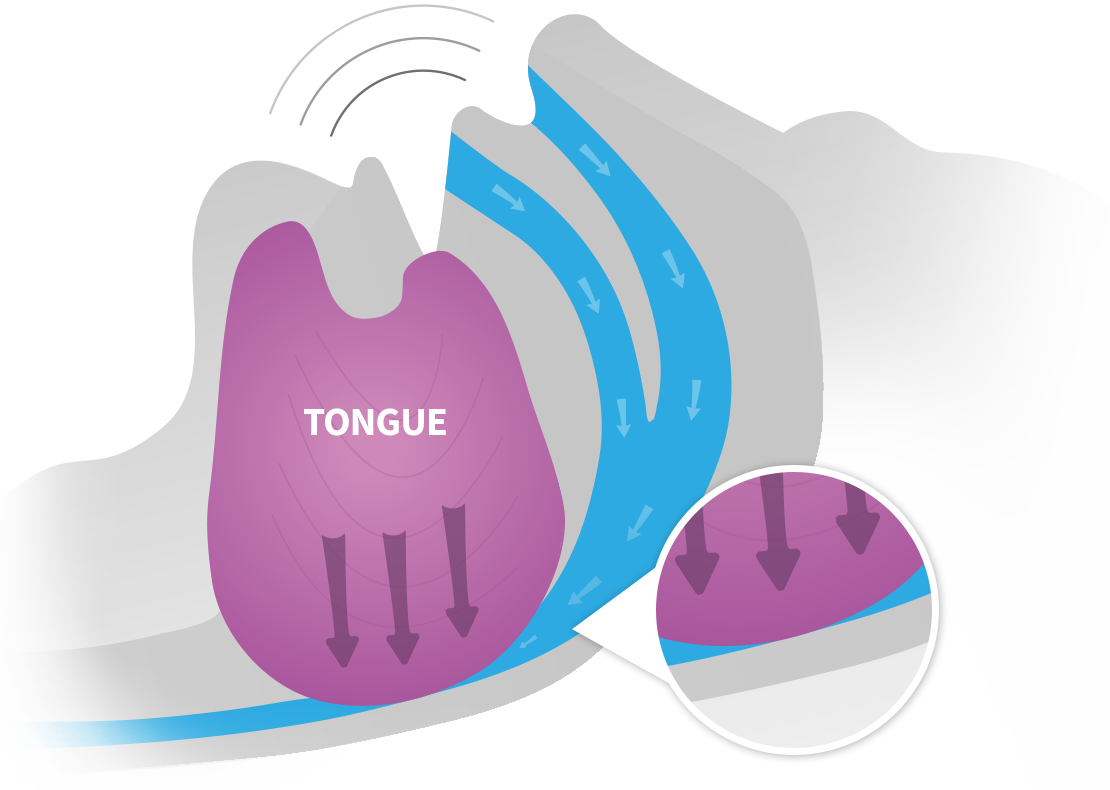
A Fatigued Tongue
Your tongue muscles are an important factor in a good night’s sleep
When you sleep your tongue and upper airway muscles relax. As you breathe, air flows past these relaxed tissues making them vibrate, creating the snore sound.
Nearly everyone snores now and then, but for
some people it can be a chronic problem.
Treatments
There are several options for treating snoring and obstructive sleep apnea
Many snoring therapies focus on creating space in the airway. NMES does something unique.
1. Nighttime treatments
Uncomfortable. not suitable for all
Mandibular (jaw) Advancement Device works by temporarily moving the jaw (and tongue) forward.
2. Surgical treatments
Invasive
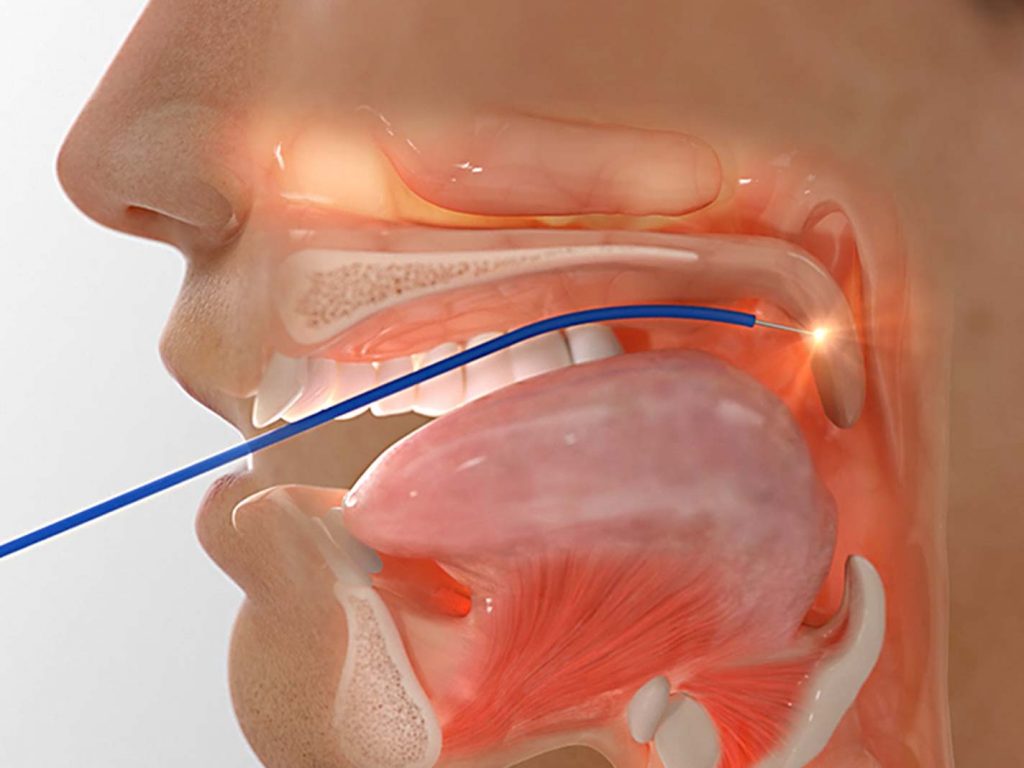
Surgery is usually an option after other treatments have failed. Examples include tissue or tonsil removal.
3. Daytime NMES therapy
Simple, effective & painless
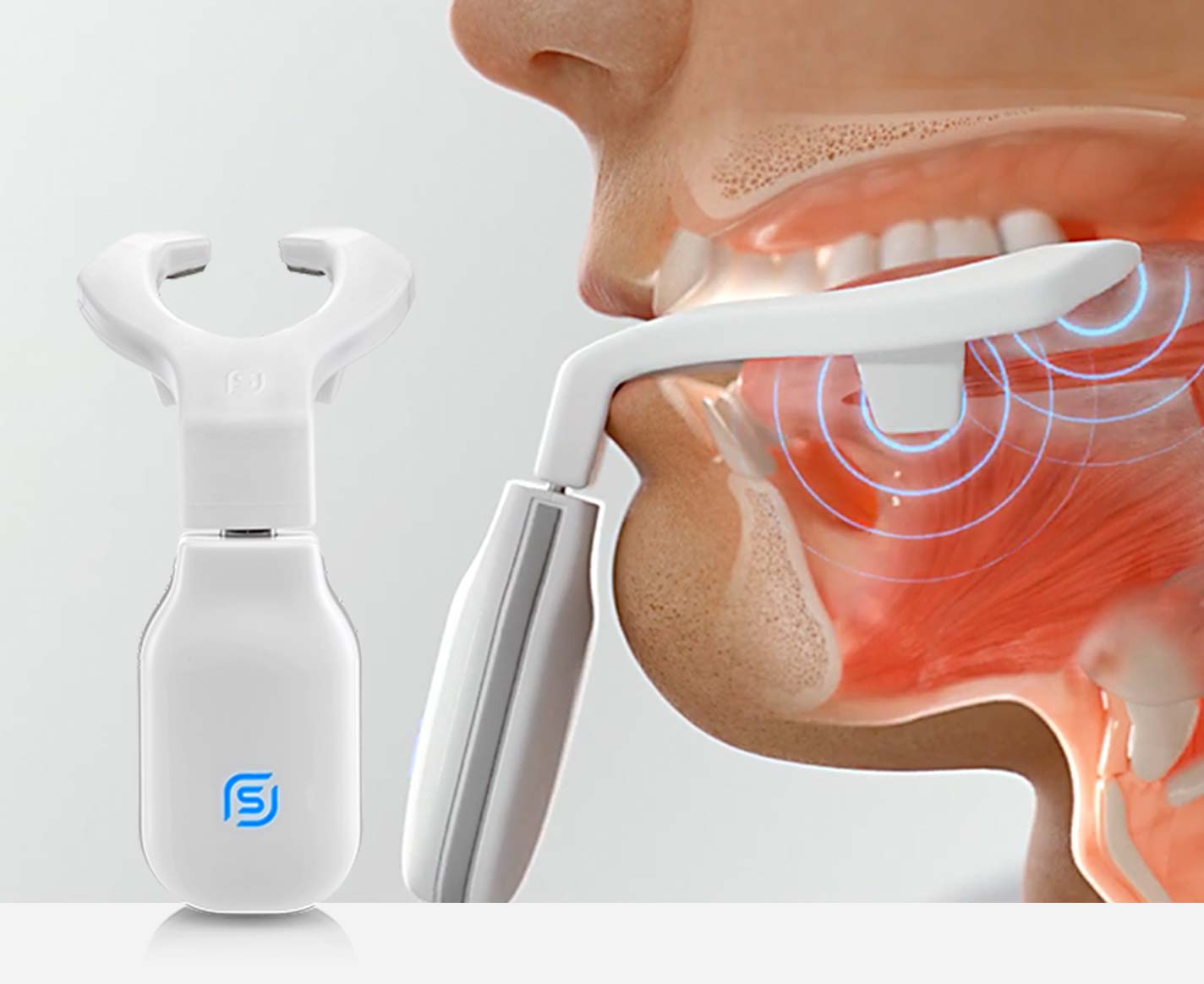
NMES physiologically retrains the upper airway and tongue, to stay in its natural position while you sleep.
A Daytime Therapy
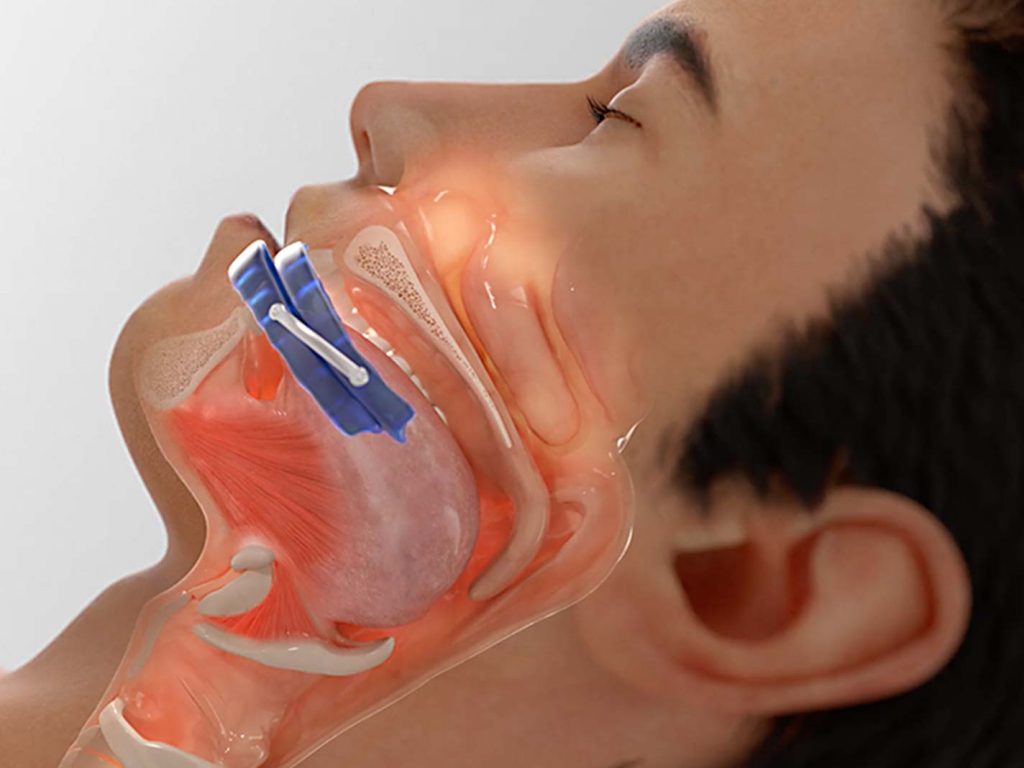
Neuromuscular electrical stimulation (NMES) with eXciteOSA for snoring
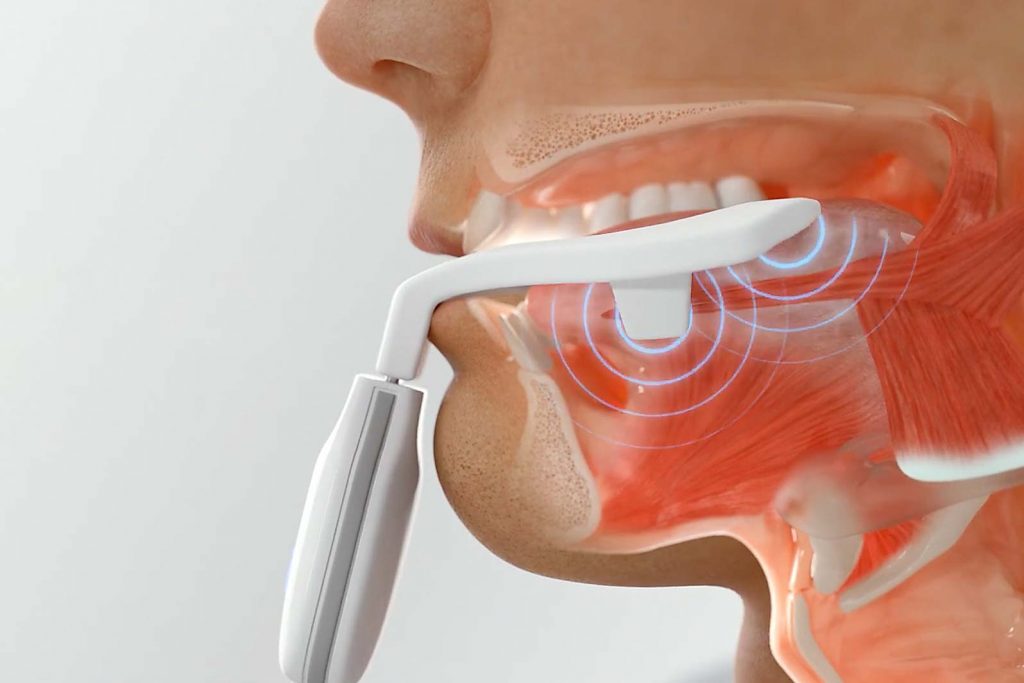
NMES safely activates nerves and trains muscles. NMES is a familiar and well-established technique in medicine and athletics.
eXciteOSA for snoring applies this same technique to training the tongue and upper airway muscles.
NMES is different
Convenient daytime therapy
Comfortable and painless leaving you with nothing to wear at night.
90% responded to therapy
Of 115 patients, 90% responded to therapy. An average 41% reduction in snoring time (>40db) was seen across all patients2.
Retrains the upper airway
Physiologically retrains the upper airway. No other device currently on the market does that.
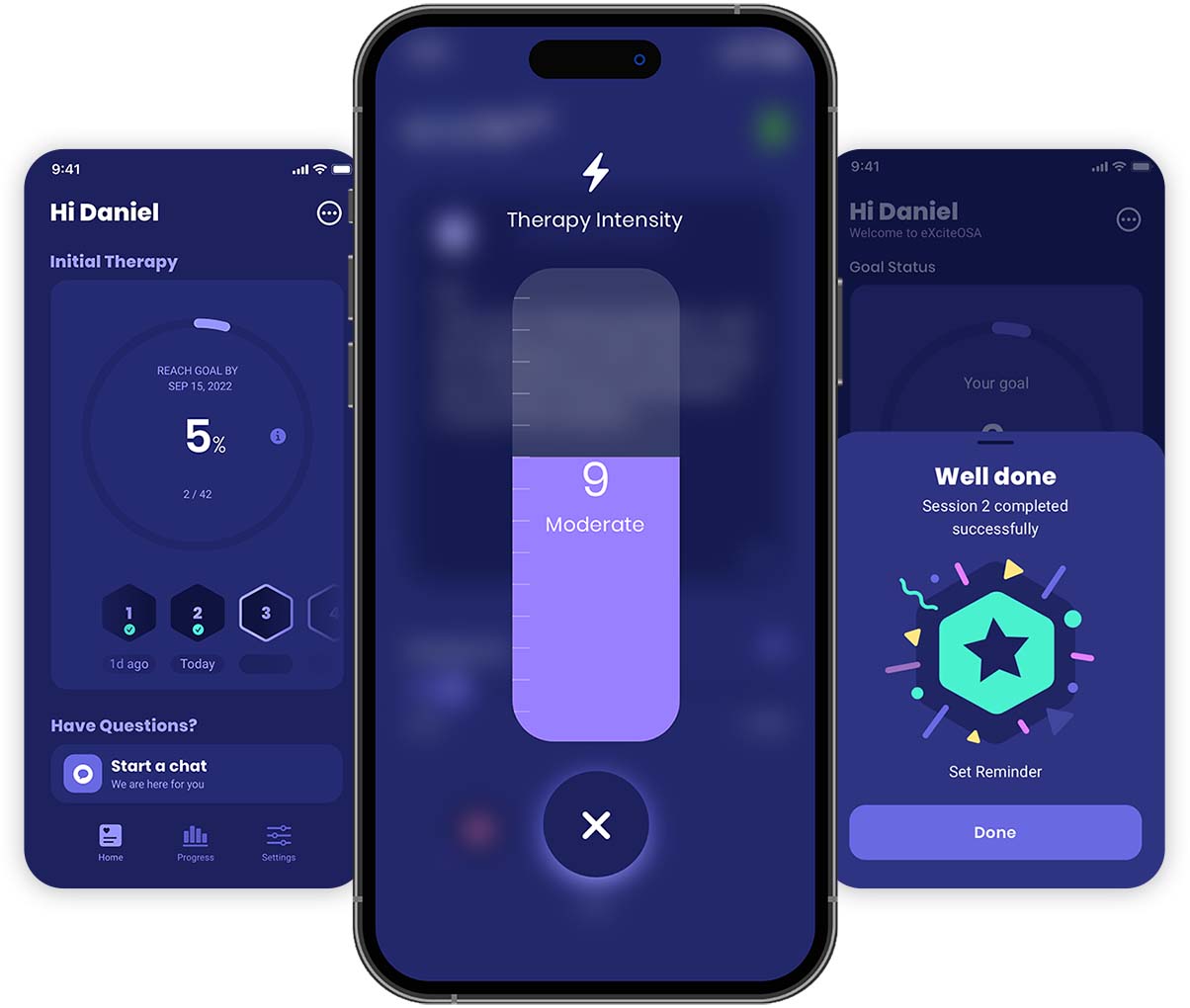
The App
You are in control
Use the eXciteOSA for snoring app to control the intensity of the stimulation and get guidance, reminders, and notifications about your therapy.

Better Sleep or your money back*
If you do not experience improved sleep after completing 70% of 42 therapies in 8 weeks, we will refund you the price of the device.
Hear how eXciteOSA® has transformed peoples sleep
“Very easy to use and quite simple to just find 20-minutes at a time.”
Trusted by Experts
Backed by leading sleep specialists
Long term snoring
It’s important to do something if you snore
Your snoring may lead to various health risks7-9 and may indicate the first stages of obstructive sleep apnea (OSA)10.
It’s not justabout you
Your snoring may be causing stress and harming the long-term health of your bed partner and other family members.

Frequently asked questions
Transcutaneous electrical nerve stimulation (TENS) machines stimulates the sensory nerves (the nerves that send signals from the body to the brain) with the purpose of disrupting the pain signal.
Neuromuscular electrical stimulation (NMES) also uses electrical stimulation, but targets the motor nerves (the nerves that send signals from the brain to the body) in order to stimulate the muscles directly.
Sensory and motor nerves fire at different frequencies, which is how TENS and NMES devices are able to impact them differently.
eXciteOSA® for snoring is a user-controllable neuromuscular electrical stimulator (NMES) that delivers a mild electrical current with defined frequencies to stimulate and improve muscle function in the mouth and tongue.
Unlike traditional snoring therapies, eXciteOSA® strengthens tongue and throat muscle tone, to prevent excessive muscle relaxation during sleep, reducing airway collapse and therefore snoring.
A daytime therapy with no night-time wearable necessary for a better night’s sleep.
There are several options for treating snoring.
Mandibular (jaw) advancement devices (MADs) work by temporarily moving the jaw forward, in order to create more space in the airway.
Surgery is usually an option to consider after other treatments have failed. Examples include removal of soft tissues from the airway, or procedures designed to stiffen the airway.
NMES physiologically retrains the upper airway and tongue to maintain the tongue’s natural position while you sleep, effectively helping your body help itself. eXciteOSA for snoring is the only device in the world that can deliver NMES directly to your tongue and surrounding soft tissue.
Risk-free trial
*The eXciteOSA Better Sleep Guarantee: Consistent use is critical to success. While we don’t expect perfection, we do ask that you complete 70% of your 42 therapies within 8 weeks of receiving your product before receiving your refund.
A session is equivalent to 20 minutes. In addition, it is recommended that you increase the therapy intensity gradually over the treatment period to ensure that you give the treatment every chance of being effective. Please note that once the initial therapy is finished and to maintain the treatment you need to use the device at least twice a week forever.
The mouthpiece is a precision piece of engineering responsible for delivering neuromuscular electrical stimulation targeted primarily at the tongue. It needs to be replaced every 3 months.
References
- Kotecha B, Wong PY, Zhang H, Hassaan A. A novel intraoral neuromuscular stimulation device for treating sleep-disordered breathing. Sleep Breath 2021;25(4):2083-2090.
- Baptista PM, Martinez Ruiz de Apodaca P, Carrasco M, Fernandez S, Wong PY, Zhang H, Hassaan A, Kotecha B. Daytime neuromuscular electrical therapy of tongue muscles in improving snoring in individuals with primary snoring and mild obstructive sleep apnea. J Clin Med 2021;10(9):1-11.
- Nokes B, Baptista PM, Martínez Ruiz de Apodaca P, Carrasco-Llatas M, Fernandez S, Kotecha B, Wong PY, Zhang H, Hassaan A, Malhotra A. Transoral awake state neuromuscular therapy for mild obstructive sleep apnea. Sleep Breath [accepted; in-press].
- Lofaso F, Coste A, Gilain L, Harf A, Guilleminault C, Goldenberg F. Sleep fragmentation as a risk factor for hypertension in middle-aged nonapneic snorers. Chest 1996;109(4):896-900
- Kalchiem-Dekel O, Westreich R, Regev A, Novack V, Goldberg M, Maimon N. Snoring intensity and excessive daytime sleepiness in subjects without obstructive sleep apnea. Laryngoscope 2016;126(7):1696-1701
- Gottlieb DJ, Yao Q, Redline S, Ali T, Mahowald MW. Does snoring predict sleepiness independently of apnea and hypopnea frequency? Am J Respir Crit Care Med 2000;162(4 Pt 1):1512-1517
- Hu FB, Willett WC, Manson JE, Colditz GA, Rimm EB, Speizer FE, Hennekens CH, Stampfer MJ. Snoring and risk of cardiovascular disease in women. J Am Coll Cardiol 2000;35(2):308-313.
- Deeb R, Judge P, Peterson E, Lin JC, Yaremchuk K. Snoring and carotid artery intima-media thickness. Laryngoscope 2014;124(6):1486-1491.
- Scher AI, Lipton RB, Stewart WF. Habitual snoring as a risk factor for chronic daily headache. Neurology 2003;60(8):1366-1368.
- Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 2002;165(9):1217-1239.